Tetrada Fallo
Author Ольга Кияница
2018-05-10
Tetrada Fallot (TF) is one of the most common congenital heart disease (IOP). It is often referred to as "blue heart defect", because with this pathology, due to a shunt from the right to the left, an insufficient amount of blood passes through the lungs, resulting in organs and tissues receiving less oxygen.
Patients with tetralogy of Fallo show cyanosis shortly after birth, so often there is early medical care.
In the Fallo tetrad, surgical intervention is carried out in a compulsory manner, or the child is inevitably threatened with death. As a rule, the operation is performed in a step-by-step manner, although recently more rapid treatment of blemishment has begun using catheter access. When a successful operation is performed, the most favorable outcome is a favorable outlook.
Video: Tetrada Fallot (Fallo). Congenital heart defects
Historical reference
For the first time he described the Stensen's Testimony of Flaws in 1672; but it was the French physician Etienne-Louis Arthur Fallot who first accurately indicated the clinical and pathological features of the defects. It happened in 1888.
Although the disorder was diagnosed fairly early, the treatment of blemish was not carried out until the 1940s. American cardiologist Helen Brook Tausig acknowledged that cyanosis is progressing and inevitably leads to the death of infants with the tetrad Fallo. She suggested that cyanosis was caused by insufficient pulmonary blood flow. Her collaboration with the American surgeon Alfred Blaylok led to the first achievements on the way of facilitating the lives of sick infants.
In 1944, Blaylock created the first Blood-Taussig shunt between subclavian artery and pulmonary artery
Bluelock-Taussig's innovative surgical technique for shunting has opened a new era in cardiac surgery for newborns.The development of the Potts shunt (from the descending aorta to the left pulmonary artery), the Glenn shunt (from the upper hollow vein to the right pulmonary artery) and the Waterstone shunt (from the ascending aorta to the right pulmonary artery).
Scott completed his first open operation in 1954. In less than half a year, Lillehei performed the first successful reconstruction of a patient with Fallot's notebook in the open heart. The following year, with the advent of cardiopulmonary bypass Gibbonsom, another historic epoch of cardiac surgery was established. Since then, numerous improvements have been introduced in the surgical technique and the preservation of the myocardium, enabling successful treatment of defects.
Description
For the tetrad of Fallot there are four peculiarities:
- Obstruction of right ventricular output department (vortex stenosis)
- Defect of interventricular septum
- Incorrect placement (dextrantion) of the aorta
- Right ventricular hypertrophy.
Sometimes an additional defect of the interstitial septum is determined, then speak of Pentade Fallo. The main violation of the tetrad is due to underdevelopment of the infundibular department of the right ventricle, which leads to a change in the anterior and lower parts of the funnel-shaped septum. This discrepancy determines the severity of the disease.
Hemodynamics at TF
Hemodynamics depends on the degree of obstruction of the outflow of the right ventricle. The defect of the interventricular septum usually does not act as a limiting factor, and the pressure in the right and left ventricles is usually aligned.
If the obstruction is severe, the flow of blood inside the heart is carried out from right to left, and pulmonary blood flow may worsen considerably. In this case, blood flow often depends on arterial duct or bronchial collaterals.
Phases of development of a vice
Depending on the severity of the disease, three phases of TF development are distinguished:
- The first one is relatively favorable. The child does not notice significant lag in development. It lasts approximately from birth to half a year.
- The second one is characterized by a syndrome of cyanotic attacks. In this phase, severe brain disorders and fatal outcomes are most often developed. It lasts from six months to two years.
- The third one is considered transient, since the clinic changes and often adopts adult features.
A bit of statistics and facts on the phallo's notebook:
- It is determined in approximately 10% of cases of congenital heart defects, that is, it occurs in 3-6 infants for every 10,000 births.
- The disease is one third of all airborne illnesses in patients under the age of 15.
- For brothers and sisters of sick parents, the incidence is 1-5%, and is more common in men than in women.
- The disorder is associated with excessive anomalies such as clefts of the lips and the palate, hypospadias, skeletal and craniofacial anomalies.
- Tetrada Fallo is also observed in other mammals, including horses and rats.
Reasons
The causes of most congenital heart defects are unknown, although genetic studies suggest multifactorial etiology.
A study conducted in Portugal showed that the polymorphism of the methylenetetrahydrofolate reductase (MTHFR) gene can be considered as the susceptibility gene of the Fallot tetrad. [1 - Lee CN; With YN; Cheng WF; Lin MT; Wang JK; Wu MH; Hsieh FJ. Association of the C677T methylenetetrahydrofolate reductase mutation with congenital heart disease. Acta Obstet Gynecol Scand. 2005; 84 (12): 1134-40]
Prenatal Factors That Increase the Risk of Tetradot's Development Fallo:
- The incidence of rubella (or other viral infections) during pregnancy
- Bad nutrition of a pregnant woman
- Drinking alcohol during pregnancy and after delivery
- Mother's age is over 40 years old
- Congenital defects from parents
- Phenylketonuria or diabetes in pregnant women.
Children with Down syndrome also have a higher incidence of Fallot tetrahedron, as are babies with fetal hydantoin syndrome or fetal carbamazepine syndrome.
Clinic
Clinical features of the phallus tetradus directly depend on the severity of the anatomical defects. The following symptoms are most commonly diagnosed in infantile patients:
- Difficulty with feeding
- Failure to develop normally
- The bluish-pale skin of the skin during crying or feeding
- Severe shortness of breath, usually worsening with age
Physical data include the following:
- The growth and weight of sick children does not correspond to the age
- Cyanosis of the lips and nail bed, which is usually expressed from the very moment of birth
- After 3-6 months, the fingers and toes become knotted (the symptom of "drum sticks")
- Nails become rounded ("symptom of watch glasses")
- Systolic noise is usually present in the front along the left sternum
Odor-cyanotic attacks
They are a sign of a severe TF. Most often it manifests itself in the interval half a year-a year, at the same time it is often noted a relative or absolute anemia.
During an attack, a severe spasm of the infundibular section of the pancreas develops, which causes the venous blood to enter the brain through the aorta, thereby causing the expressed hypoxia of the central nervous system. The amount of oxygen in the blood during an attack is 35% and below. Hearing before this noise almost completely disappears.
At first the development of the attack is determined:
- Anxiety and strong fright
- Extended pupils
- Increasing blistering of the skin and mucous membranes
- Increasing shortness of breath
After these signs, there is fainting and cramps.
Such attacks can end in 10-15 seconds or 2-3 minutes, after which the patient is determined by lethargy and adynamicity. If enough of the pulmonary collaterals develops to 4-6 years, then the attacks develop less or go away at all. In severe cases, paresis or other violations of brain activity arise. Also, the risk of death is high with the development of the attack.
Diagnostics
In patients with significant cyanosis, combined with a tendency to bleeding, the following changes are determined:
- Reduction of blood coagulation factors
- Low platelet count
- Reduced coagulation rates
- Reduced total fibrinogen
- Extended prothrombin time and coagulation
When analyzing arterial blood, the following is determined:
- Normal or reduced oxygen saturation
- The pH and partial pressure of carbon dioxide (pCO2) are normal unless the patient is in critical condition
From instrumental research methods are used:
- Echocardiography
- Roentgenography of the chest
- Magnetic resonance imaging
- Catheterization of the heart (in extreme cases)
Echocardiography in conjunction with Doppler provides the following data:
- It accurately diagnoses arterial duct or a defect of the interstitial septum
- With some degree of accuracy, coronary lesions are determined
- Valve changes are easily detected
In many settings, echocardiography is the only diagnostic study used prior to surgery.
Video: Tetrada Fallo
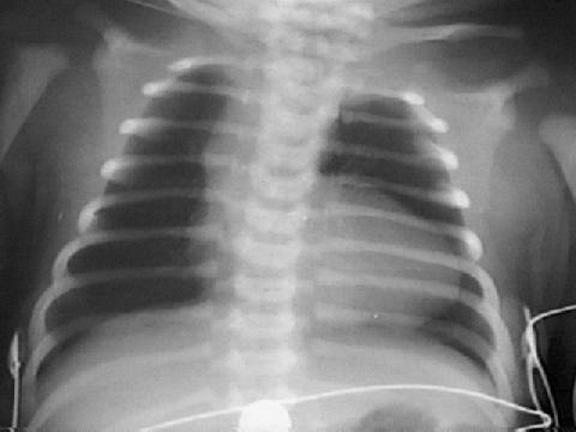
X-ray of the chest provides the following indicators:
- Decrease of vascular pattern in the lungs
- The classic form of "boot heart" (coeur en sabot) is a hallmark of heart disease.
MRT allows you to determine:
- Clear location of the aorta, pulmonary artery and its branches
- The state of the intestinal and inter-parietal septum, the thickness of the wall of the right ventricle
- The magnitude of intracardiac pressure, gradients and blood flow
Cardiac catheterization can be beneficial in any of the following cases:
- The anatomical structure of the heart and adjacent vessels can not be fully determined by echocardiography
- The current pulmonary artery disease causes great disturbance
- Pulmonary or arterial hypertension is determined
After catheterization of the heart, results such as the size of the pulmonary ring and the pulmonary arteries, the severity of the stenosis of the withdrawal part of the prosthesis, the location and size of the accompanying anomalies and defects can be provided.
Treatment
In severe cyanosis, the following therapies are used:
- The child should be put on the shoulder of the mother, while pulling it with his knees. It provides a calming effect, reduces venous outflow and increases systemic vascular resistance
- Oxygen is used in a limited amount, as the heart anomaly contributes to the reduction of pulmonary blood flow
- The introduction of morphine sulfate intramuscularly or subcutaneously can reduce the ventilation dynamics and systemic venous outflow
- Phenylephrine is used to increase systemic vascular resistance
- Dexmedetomidine infusion is used, but with caution and taking into account titration rules
General anesthesia is the last resort in rendering quick help to a patient with pronounced cyanosis at Fallot's tetrad.
Most infants with TF require a suitable surgical treatment. Surgery is preferably carried out at the age of about 12 months. Primary correction is an ideal operation and is usually performed in the presence of a cardiopulmonary bypass.
Palliative procedures (for example, the placement of a modified Blalock-Taussig shunt) may be necessary for patients with contraindications to primary rehabilitation, which include the following:
- The presence of abnormal coronary artery
- Very low birth weight
- A small network of pulmonary arteries
- Multiple accompanying intracardiac anomalies
Forecast
An early operation is not shown to all children with Fallot's tetrad, although without a surgical intervention, the natural progression of blemish often has a poor prognosis.
Progression of the violation depends on the severity of the stenosis of the outgoing department of the right ventricle
In the current epoch of cardiac surgery, children with simple forms of tetrad Fallo have a good long-term survival with excellent quality of life. Only in some cases, the maximum capacity for physical activity is reduced.
Sudden death from ventricular arrhythmias develops in 1-5% of patients at a later stage of life, and the cause remains unknown. It was supposed that dysfunction of the ventricles could help.
In the absence of treatment, patients with tetrad Fallo face additional risks, which include paradoxical embolism leading to stroke, pulmonary embolism, and bacterial endocarditis. It is well-known that children with congenital heart disease are prone to stroke. In most of these children, the causes of stroke were associated with thromboembolism, prolonged hypotension / anoxicemia and polycythemia. It is often forgotten that residual shunts or oval holes also contribute to the development of stroke.
Without surgical intervention, mortality is gradually increasing: from 30% at the age of 2 years to 50% at the age of 6 years. Mortality is highest in the first year of life, and then practically does not change until the second decade. It is assumed that in such cases, no more than 20% of patients reach the age of 10 years, and less than 5-10% of patients survive until the end of the second decade.
In most patients who live up to 30 years of age, congestive heart failure develops, although in the presence of shunts causing a minimum hemodynamic disorder, they can reach normal life expectancy. Also reported cases of survival of patients under the age of 80 years. Due to the use of advanced surgical methods for the period from 1979 to 2005. the death rate associated with Fallot's tetrad is down by 40%. [2 - Pillutla P; Shetty KD; Foster E. Mortality associated with adult congenital heart disease: Trends in the US population from 1979 to 2005. Am Heart J. 2009; 158 (5): 874-9]
If tetrad Fallo is combined with pulmonary atresia, then the worst predictions are given. In such cases, only 50% of patients survive up to 1 year and 8% can reach the age of 10 years.
Video: Elena Malysheva. Tetrada Fallot is a congenital malformation of the heart
Similar articles

In many cases, the development of severe heart disease can be prevented through exercise. Most of the leading experts in the field of cardiology are confident that heart training should be an integral part of a healthy lifestyle. In this case, doctors prescribe specific exercises even for patients suffering from cardiopathology.

No one is immune from a heart attack, but since this critical condition most often develops in people of middle and old age, it is this category of population that needs to be especially vigilant. It is useful to know the signs of myocardial infarction and the actions that must be performed to provide emergency care.

One in 120 babies is born with a heart malformation. Some of them are heavy, but in most cases, they do not represent danger. Defects may include abnormal walls or heart valve shapes, as well as blood vessels that fit or depart from the heart.
