Treatment of antidromic tachycardia
Author Ольга Кияница
2018-01-18
Antidromic tachycardia is one of the hereditary diseases of the cardiovascular system. In ICD-10 is considered under the syndrome of premature ventricular excitation. In the formation of pathology involved the bundles of Kent, which are called complementary and directly participate in the formation of arrhythmias in the type of reentry.
Tachyarrhythmia is rare. Patients with signs of a rapid heartbeat often seek urgent help, after which the presence of additional pathways and, as a consequence, WPW syndrome are identified.
During the course of the disease, there are minimal risks of sudden death, but the correct drugs should be prescribed.Otherwise, the state of health of the patient may deteriorate.
Video New possibilities for treating ventricular tachycardia
Medicinal treatment of antidromic tachycardia
During development of antidromic tachycardia, there are wide ventricular complexes formed as a result of overexcitation of the cardiac muscle. Against the background of such changes, there is a high frequency of cardiac contractions, a pronounced clinic, a violation of hemodynamics. Such signs have unfavorable prognostic significance, therefore immediate medical intervention is required.
Basic tactics of management of patients with antidromic tachycardia:
- For the first time, the attacks have first been stopped by cardioversion, which, at the first charge, is 100 Дж. When it is ineffective, medication therapy is used.
- If the patient is well tolerated by an attack or the clinic is not strongly expressed, then the medication is prescribed.
The basis of the medical treatment of antidromic tachycardia is those preparations that prolong the refractory period of the pathological pathways. Such agents are amiodarone (cordarone) and novocainamide. Under the action of blocking substances there is an overexcitation of the ventricles, which reduces the risk of sudden death.
Amiodarone - shown in patients who, in addition to tachyarrhythmia, have structural changes in the heart. It is administered intravenously with a maximum loading dose in the first 20 minutes and then in less amount during the day.

NovoKainamide - is prescribed to a patient without an organic pathology of the heart. It is administered intravenously until the attack of tachyarrhythmia is stopped. Also, the drug ceases to enter in the event that the pressure decreases, the width of the ventricular complexes increases by half from the initial one.
There are drugs that are contraindicated for use in the development of antidromic tachycardia:
- Digoxin, beta-blockers, verapamil-disrupt pulses through the atrioventricular node and thus contribute to their passage through pathological channels, which can cause an increase in the frequency of heart rate and the development of ventricular fibrillation.
- Lidocaine is not used due to the lack of properties for lengthening the refractory period of the pathological canal. With excessive ventricles, the drug may cause an increase in the frequency of their contractions, especially in the context of atrial fibrillation.
For prolonged antiarrhythmic therapy, preparations of IP and class III are used. According to international recommendations, propafenone and flekainid are commonly used today, as well as amiodarone and sotalol. The efficacy of amiodarone does not always prevail over the side effects of the drug, so if the doctor can recommend a drug with a milder effect, then it's worth not using the remedy. An exception is made up of patients with concomitant organic pathology of the heart.
In a number of cases, the long-term use of antiarrhythmic drugs in the WPW syndrome is quite possible. In particular, when determining with the help of an ETI an additional channel that is not capable of fast transfer of impulses.
Interventional treatment of antidromic tachycardia
It is an alternative therapeutic way of medication. Today, radiofrequency catheter ablation, which is increasingly carried out in comparison with operations in the open heart, is the leading position.
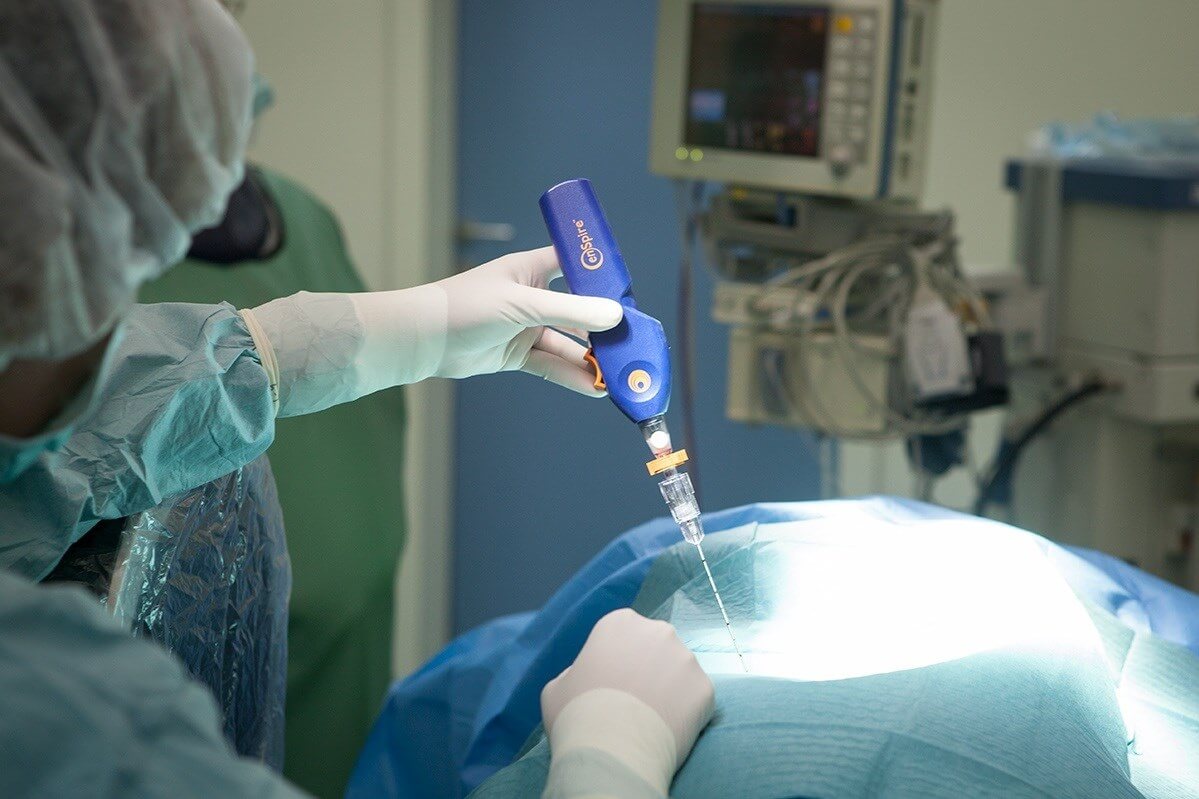
RFA is most often shown to patients with clinical signs without severe hemodynamic disturbances. Also, the method is used in the case of negative heredity, asymptomatic pathology, or in the presence of hidden additional paths. The last indication basically corresponds to the patient's preference. After the first destruction of the pathological channel, the result is observed in 95% of cases. The remaining 5% are recurrent seizures, and tissue swelling may also occur in the affected area. For the second holding, the efficiency is almost 100%.
Participation of the patient in the treatment of antidromic tachycardia
For all patients with WPW syndrome, it is important to know how and why this pathology develops. This will help to behave correctly in the process of treatment, which is especially relevant for young people who do not have a clinic.Such patients, as a rule, learn about overexcitation of the ventricles by accident, for example, during a preventive examination. Therefore, it is extremely important that there is a realization that it is necessary to take regular examinations at the doctor, not delay with the appeal for help when the first signs appear.
If there is an overexcitation of the ventricles, you should wear the latest last electrocardiography supplemented by a medical report.
Patients with antidromic tachycardia can not compete in sports. It is also recommended that the relatives of the patient undergo a screening examination and, if necessary, appoint appropriate treatment for rhythm disturbance.
