Hypertensive angina
Author Ольга Кияница
2019-02-02
Angina pectoris is an acute coronary disease, which most often manifests itself as a back pain. Other symptoms may also be determined, whereas the same disorder is often combined with other pathologies. In particular, it is quite often possible to hear among patients about hypertonic angina, which in the course of its development manifests itself as signs of two complicated diseases.
Hypertensive angina is a clinical syndrome that is not encountered in medical interpreters and international classifications, but points to the joint development of hypertension and angina in one patient.
For the diagnosis of hypertensive angina pectoris use standard methods for investigating the cardiovascular system - ECG, echocardiography, angiography. The treatment scheme depends on the severity of the manifestations, the accompanying pathologies, and the dynamics of the disease.
Video: Angina And High Blood Pressure What Are The Symptoms Of Angina High Blood Pressure
Hypertension and angina pectoris
Patients with systemic hypertension suffer from diseases of the coronary arteries caused by coronary microvascular dysfunction. Structural coronary microvascular disorders such as capillary depletion (rarification), functional changes and endothelial dysfunction are common causes. In addition, in postmenopausal women with hypertension, the deficit of the microvascular channel can also play a key pathogenetic role in the development of angina pectoris.
A general idea of the relationship between hypertension and angina pectoris
Among patients with systemic hypertension, typical abnormal chest pain is relatively common, a positive response to stress testing and angiographically normal coronary arteries. Functional and structural mechanisms affecting coronary microcirculation are often the cause of microvascular angina in patients with hypertension.
Capillary deficiency and left ventricular hypertrophy are common structural disorders responsible for microvascular dysfunction with hypertension.
Among the functional disorders that also contribute to the appearance of microvascular angina, insulin resistance is of particular relevance. This pathology often leads to endothelial dysfunction and estrogen deficiency in women in the postmenopausal period. Also, women who have undergone hysterectomy (uterus removal) are at risk.
A higher incidence of microvascular angina is observed in women than in men. Its association with menopausal status (approximately 70%) has led to the assumption that the estrogen deficiency (female hormone) may play a pathogenic role in the subgroup of women in peri-and postmenopausal conditions when stenocardia and hypertension [1 - Kaski JC, Rosano GM, Collins P, Nihoyannopoulos P, Maser A, Poole-Wilson PA. Cardiac syndrome X: clinical features and left ventricular function. Long-term follow-up study. J Am Coll Cardiol. March 15, 1995; 25 (4): 807-14].
A similar situation is observed with arterial hypertension, the incidence of which in women after menopause increases significantly. The link between estrogen deficiency and the development of microvascular angina and hypertension is rather complicated. It includes endothelial dysfunction, altered responses of the autonomic nervous system, and activation of the renin-angiotensin-aldosterone system (RAAS) [2 - Lima R, Wofford M, Reckelhoff JF. Hypertension in postmenopausal women. Curr Hypertens Rep. 2012 Jun; 14 (3): 254-60].
Patients with arterial hypertension and angina often have a slow course of the disease and tortuous coronary arteries, which may be thought to be due to "obstruction" of small vessels.

Pathogenesis of hypertensive angina pectoris
Mechanisms underlying angina pectoris in patients with essential hypertension without obstructive coronary artery disease are still largely unknown. Several functional pathophysiological anomalies have been reported in these patients, which are as follows:
- Endothelial dysfunction.
- Increased sympathetic tone.
- Microvascular spasm.
- Estrogen deficiency.
- Psychological disorders.
- Increased sensitivity to pain.
In addition, with hypertonic disease, a higher probability of manifestation of metabolic syndrome, such as dyslipidemia, obesity and insulin resistance, is detected in comparison with the general population (30% versus 8%, respectively) [3 - Agrawal S, Mehta PK, Bairey Merz CN. Cardiac Syndrome X: update 2014. Cardiol Clin. Aug. 27, 32 (3): 463-78]. This happens more often in women in the postmenopausal period. As a result, insulin resistance can be an important mechanism for the development of vascular dysfunction. Additional impacts are structural anomalies of the type of capillary rarefaction, as well as medial hypertrophy and / or arteriolar vascular fibrosis.
Many studies have determined that myocardial ischemia is due to functional and / or anatomical disturbances in coronary microcirculation. There is also a relationship of pathology with changes in the pH of the coronary sinus and / or the development of myocardial lactate during stimulation or stress-induced changes in cardiac high-energy phosphate.
In the study of pathogenesis of hypertensive angina pectoris used methods of perfusion of myocardium radionuclides, measurement of oxygen saturation of the coronary sinus and magnetic resonance spectrometry. Additionally, it has been shown that both coronary microvascular spasm and / or the decrease in the capacity of the microvascular vasodilatator causes myocardial ischemia and anginal symptoms characteristic of arterial hypertension and angina pectoris.
Video: Nursing Review on the Cardiac System, Hypertension, Angina and CHF
Hypertensive angina in women
In women in the peri-and postmenopausal period with hypertension, the cessation of ovarian function and, consequently, estrogen deficiency (female hormone) play a major role. The deficiency of estrogen negatively affects the cardiovascular system, contributing to the development of heart and vascular diseases.
The deficiency of estrogen is associated with the loss of the direct protective effect of the hormone in the vessel wall and indirectly with the negative changes in some other traditional risk factors for coronary heart disease. As a result, cellular resistance to insulin occurs, cholesterol in the blood increases and body weight increases.
Estradiol 17β has the properties of blocking calcium channels, thereby acting as an endothelium-independent vasodilator. Consequently, loss of estrogen negatively affects both the dependent and estrogen-independent vasodilatation.
Subsequently, there are prerequisites for increasing arterial pressure, causing arterial hypertension and coronary vasomotor reaction. Thus, estrogen deficiency is one of the most important mechanisms leading to the development of arterial hypertension in women in the postmenopausal period.
Interestingly, the deficiency of estrogen has a negative effect on the occurrence of chest pain in women with heart syndrome X (CKD). Low levels of estrogen are associated with a violation of the function of the endogenous opioid system and the gamma-aminobutyric acid system (GABA). As a result, low concentrations of estrogen reduce or suppress the development or release of endorphins and enkephalins, which leads to an increase in perception of pain.This mechanism was confirmed by the fact that the introduction of estrogen removes chest pain in patients with CKD.However, hyperreactivity of heart pain receptors, abnormal transmission and / or modulation of pain signals at the subcortical level, or a variable combination of all these abnormalities can equally lead to abnormal activation of certain areas of the brain, as well as to the reduction of the pain threshold and psychological instability.
Traditionally, the prognosis in patients with hypertensive angina was considered favorable. However, a study on the evaluation of ischemic syndrome in the female group has shown that women with permanent chest pain have a twofold increase in cardiovascular complications. In particular, non-fatal myocardial infarction, stroke, congestive heart failure, and death from cardiovascular disease often occur in comparison with patients without this disease [4 - Johnson BD, Shaw LJ, Pepine CJ, Reis SE, Kelsey SF, Sopko G, Rogers WJ, Mankad S, Sharaf BL, Bittner V, Bairey Merz CN.Persistent chest pain predicts cardiovascular events in women without obstructive coronary artery disease: results from the NIH-NHLBI-sponsored Women's Ischaemia Syndrome Evaluation (WISE) study. Eur Heart J. 2006 Jun; 27 (12): 1408-15].

Symptoms of hypertensive crisis and angina pectoris
The clinical picture of the disease depends on the amount of damage to the heart muscle due to a violation of microcircular circulation and blood pressure.
As in a hypertensive crisis, as well as in angina pectoris, breast pain is most important. Its appearance is primarily associated with cardiovascular disease. By the nature of manifestation , rebound pain can be burning, squeezing, compressing, spreading to other parts of the body (throat, left arm, lower jaw, back) and without spread.
Additionally, in the hypertensive crisis, the following symptoms appear:
- Severe headache, especially in the area of temples and forehead.
- Weakness and dizziness.
- A sharp rise in blood pressure (normally in an adult 120-130 / 80-90).
- Redness of the skin, especially the face.
- The participation of a pulse (normally in an adult 60-90 beats / min.).
With angina can be determined:
- Feeling of a lack of air.
- Frequent heartbeat.
- Decrease in working capacity.
- Feelings of fear and panic.
As a rule, with an increase in arterial pressure and the appearance of rebound pain, the heart disease is suspected at once. Appropriate studies must be conducted to determine the exact diagnosis.
Diagnosis of hypertonic angina
The presence of endothelial dysfunction in patients with arterial hypertension and microvascular angina is confirmed by the following tests:
- Decreased coronary blood flow response to acetylcholine or atrial stimulation.
- Inadequate endothelial vasoconstrictor activity , mainly mediated by the production of endothelin-1 (ET-1) [10].
Elevated concentrations of ET-1 in plasma have been reported in patients with angina pectoris. In particular, it has been shown that they are associated with coronary microvascular dysfunction. In addition, it has been found that ET-1 increases coronary blood flow in patients with CKD in response to atrial fibrillation. However, other studies have shown a violation of the expansion of coronary microvessels in response to endothelium-independent stimuli such as adenosine, dipyridamole and papaverine, indicating primary anomalies in smooth muscle cells of vessels that can lead to vasodilatation dysfunction and spasm.
Echocardiography with coronary angiography is used to diagnose both coronary and peripheral microvascular dysfunction in patients with hypertonic disease and chest pains. In this case, as a rule, normal coronary angiograms are determined and there is no hypertrophy of the left ventricle.
Although violations of the function and structure of the microvessels are generally considered to be the consequence of high blood pressure, there is evidence that microvascular changes, that is, the depletion of capillaries and endothelium dysfunction, may be a precursor to the clinical origin of arterial hypertension. This is confirmed by the discovery of a decrease in the density of capillaries in patients with borderline hypertension and even in normotensive children suffering from hypertension, as well as in the presence of endothelial dysfunction in normotensive children with hypertension.
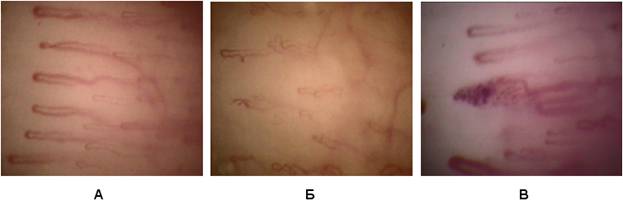
Angioarchitectonics of the capillary channel of eponymy (U. x200). And - the norm. B - vacuum of the capillary network (rationalization). B - destruction of the capillary (3 days after the hypertensive crisis)
Treatment of angina in patients with hypertension
Reliable principles for the treatment of hypertensive angina are still absent. This is partly due to a vague understanding of the pathophysiology of the syndrome and partly due to insufficiently robust randomized controlled trials conducted in the group of these patients.
The comprehensive preventive program includes recommendations for changing lifestyles. In particular, the great influence on the course of the disease has:
- Diet
- Physical activity.
- Weight loss.
- Smoking cessation.
- Decision of behavioral and psychosocial problems.
With the help of these adjustments, it is possible to positively improve the function of the endothelium and to eliminate microvascular dysfunction.
Weight loss in postmenopausal women with hypertension and angina pectoris is an important goal due to the positive effects of weight loss, both on blood pressure and on insulin resistance.
ACE inhibitors are most often prescribed when combined with hypertension and angina pectoris. These remedies have a beneficial effect on blood pressure, endothelial function and ischemia caused by physical activity. In addition, ACE inhibitors can counteract the hyperactivity of RAAS observed in patients with arterial hypertension, especially in the subgroup of postmenopausal women, and in women with cardiac pathologies.
It has been shown that beta-blockers reduce the frequency and severity of angina and improve the tolerability of physical activity in patients with cardiac disorders. New-generation beta-blockers, which have a positive effect on NO release, such as carvedilol and nebivolol, are often more effective.

First aid for angina and hypertensive crisis
Simultaneous determination of the patient's symptoms as a hypertensive crisis, and angina pectoris involves the direction of effort in the following directions:
- To create a calm atmosphere for the patient.
- Locate the patient comfortably.
- Ensure fresh air is supplied.
- Shelter your legs or attach a warmer to the legs.
- Give a dose of the drug that the doctor prescribed for the treatment of hypertension.
- Give a tongue a tablet of nitroglycerine or another drug that was prescribed by your doctor to treat angina pectoris.
In non-urgent cases, chest pain passes in a few minutes, and after complete normalization of the condition, you can return to light work. The only thing about an onset of an attack should be reported to the attending doctor, who, if necessary, adjusts the treatment schedule.
The duration of re-pain for more than 20 minutes is a sign of the development of myocardial infarction. In such cases, it is necessary to seek medical assistance without any delay.
Conclusion
Systemic hypertension is often associated with angina pectoris. Several pathogenetic mechanisms have been identified, in particular, when combining these diseases, the dysfunction of the microvascular channel of the myocardium is determined. Based on the identified cause of the disease, the most appropriate treatments are developed.Microvascular dysfunction should be subjected to careful examination, in case of need treatment. It can be determined not only in patients with systemic hypertension and angina, but also in angiographically normal coronary arteries.
Video: What is Angina Pectoris? Causes, signs and symptoms, Diagnosis and treatment
Similar articles

A pronounced clinic and a long process of development is characterized by angina, formerly known as "chest frog". The disease has specific symptoms that allow faster and accurate diagnosis of the pathology. When performing the patient's medical recommendations, stable angina is characterized by a favorable flow.

Angina common today is of various forms, but one of the most unfavorable is progressive angina. This disease may be complicated by myocardial infarction, so it is extremely important to know what the disease is.

Angina is most often manifested by pain in the heart or behind the sternum. At the same time there are additional symptoms indicating a violation of the coronary circulation. When identifying them, it is important to know what to do.
