Hypertonic arrhythmia
Author Ольга Кияница
2017-11-10
Essential hypertension, or hypertension, occurs in about 45% of individuals after 60 years of age. The disease is characterized by the constant flow and development of various concomitant clinical conditions. Hypertensive arrhythmia is one of the complications that occurs at the initial stages of the development of the underlying disease, as more severe conditions prevail in severe stages - myocardial infarction, angina pectoris, heart failure, revascularization of the coronary arteries.
In some cases hypertonic arrhythmia may be the only symptom on the background of asymptomatic occurrence of the underlying disease.
Violation of the heart rhythm is more noticeable than the raised blood pressure. Moreover, far from all elderly people have tonometers, that is, devices that measure blood pressure. That is why it is not necessary to ignore such harmless at first sight symptom, as hypertonic arrhythmia. It is dangerous whether this state itself will be considered in more detail.
Description of hypertonic arrhythmia
Arrhythmia should be understood as a violation of normal cardiac activity, which is expressed in a regular sinus rhythm.The pathogenesis of the disease consists in breaking the conductivity of the electrical impulse, as well as the presence of organic disorders in the cardiac muscle. The last version of the mechanism of development is most common in hypertonic arrhythmia.
Hypertensive disease is a very insidious disease, as in the course of its development affects many different so-called target organs: the kidneys, the optic nerve, the vascular system of the brain and the heart. Therefore, during hypertension, it is observed:
- initially high cardiac output;
- myocardial infarction as a result of revascularization of the coronary arteries.

As a result of such processes, the cardiac muscle for some time compensates for the negative effects of elevated blood pressure. After expenditure of resources begins to appear failures of the heart and hypertonic arrhythmia in this case, we can say, "the first swallow" of further complications.
The occurrence of hypertonic arrhythmia is an unfavorable symptom that indicates the initial development of organic lesions of the vessels and cardiac tissue.
Symptoms of hypertonic arrhythmia
During arrhythmia, a malfunction of the normal activity of the heart occurs, which is expressed by the following symptoms:
- frequent or slow heartbeat;
- sensation of "stopping heart" or "fading of heart";
- pain or tingling in the heart region;
- an interruption event occurs suddenly.
Signs of arrhythmia, as a rule, are combined with symptoms of heart failure in hypertension. It can be not only an increase in blood pressure, but also weakness, frequent fatigability, noise in the ears, flies in front of the eyes. Odor, swelling will indicate an initial failure of the left ventricle.
Causes of hypertonic arrhythmia
You can conventionally divide into primary and secondary. The primary concern is the presence of hypertonic disease. It is this pathology that is the root of a later complication in the form of hypertonic arrhythmia.
Secondary causes are all factors that contribute to the development of the root cause - hypertension. Therefore, if you want to get rid of arrhythmia, you need to be active in terms of eliminating predisposing conditions, which are:
- bad habits in the form of smoking;
- elderly (in men from 55 years old, and in women from 65 years old);
- disorder of lipid metabolism;
- abdominal obesity;
- increase in blood C-reactive protein;
- genetic predisposition.
In some cases, as it is with heredity and elderly age, it is difficult to make any adjustments. But with a violation of lipid metabolism, the detection of CRB in the bloodstream and smoking, you can take the necessary measures to improve the body.
There are predisposing factors contributing to the occurrence and complication of hypertensive arrhythmias. These include psycho-emotional stressful situations, lack of physical activity, lack of trace elements (calcium, magnesium), excessive intake of salt and salty products. Some women during pregnancy complicate hypertension with arrhythmia, which is usually followed by adherence to medical recommendations after delivery.
Types of arrhythmias that arise with hypertension
It can manifest itself in various forms, some of which are more dangerous than complications. We present the following arrhythmias that are most commonly encountered with hypertension in the increasing degree of severity and severity of the clinical picture:
- sinus tachycardia;
- extrasystole;
- paroxysmal tachycardia;
- blockade of cardiac activity;
- atrial fibrillation;
- atrial fibrillation and ventricles.
Sinus tachycardia
With this pathology, a rapid heartbeat is observed while maintaining sinus rhythm. The heart rate is 90 times or more per minute. With a sharp increase in blood pressure, which is often observed in a hypertensive crisis, an attack occurs in the tachycardia, which, in mild cases, goes on its own. If hypertension develops heart failure, then sinus arrhythmia may be permanent.
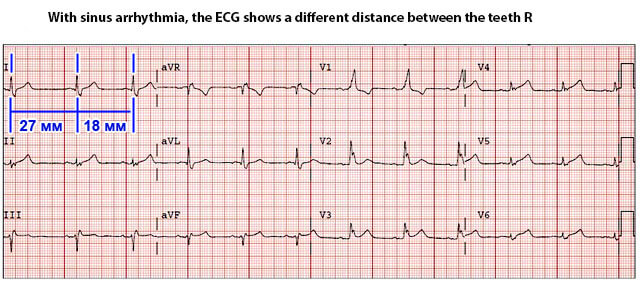
Extrasystole
It manifests itself as a feeling of "breakdown" or a severe blow for the sternum. The ECG is seen as a premature contraction. It is safer to have a single extrasystole, which in difficult cases can become steamy, polymorphic. With frequent occurrence considerably deteriorates coronary blood flow, which at hypertension and so functions not on 100%.
The place of the emergence of extrasystole (in the ventricles, atria, atrioventricular node, sinus node) also plays a role in the development of the clinical picture. The most dangerous are those hypertonic arrhythmias that develop in the ventricles, because then hemodynamics are the most rapidly disrupted. Basically, with extrasystole, the prognosis is favorable, unless significant organic damage to the heart occurs.
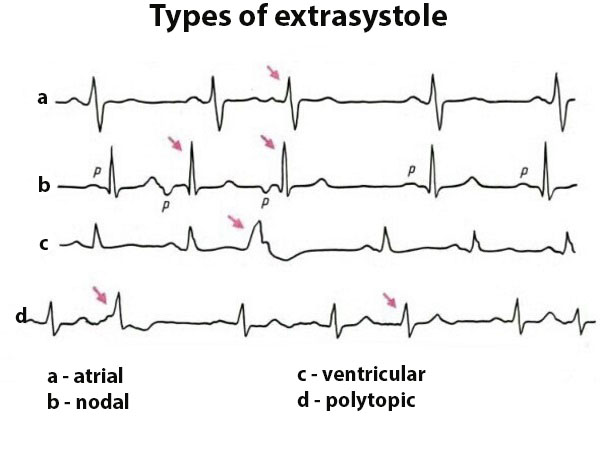
Paroxysmal tachycardia
Attacks of the heart palpitations with heart rate from 150 to 280 times per minute. Characterized by a sudden start and end of attacks. It may occur in different parts of the heart, therefore, secretes the atrial, ventricular and atrial ventricular paroxysmal tachycardia. Connected with a violation of the electrical pulse, in some cases, there are organic changes in the myocardium.
In the mild stages of manifestation goes on its own. Either for the relief of an attack, stimulate the wandering nerve. For this massage movements the carotid sinus region is rubbed or a sharp exhalation is made. Inappropriate effectiveness of these actions is taken by anaprilin or injected isoptin injected. In severe cases, electropulse treatment may be required.
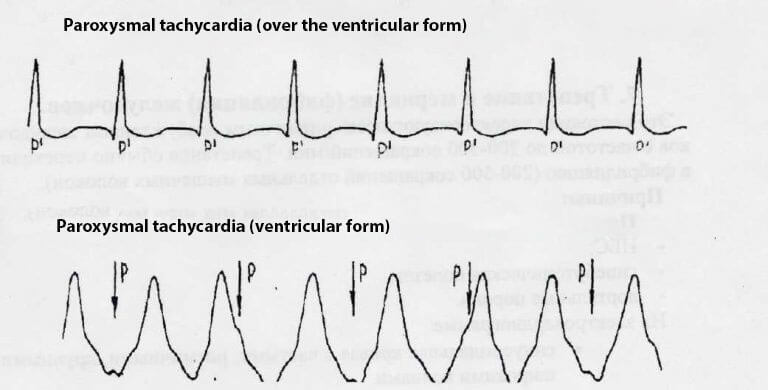
Blocks of cardiac activity
They represent a violation of the conducting system of the heart, which develops a complete or partial dysfunction of the individual parts of the organ. Often associated with organic disorders occurring in the myocardium against the background of hypertonic disease.
Heart blockade is clearly visible on the electrocardiogram. Depending on the localization of the cause of the disorder, a complete atrioventricular, sinauricular, intra-peristal blockade are isolated. The most dangerous is the complete type of blockade, since the heart begins to chaotically shrink, which negatively affects hemodynamics.
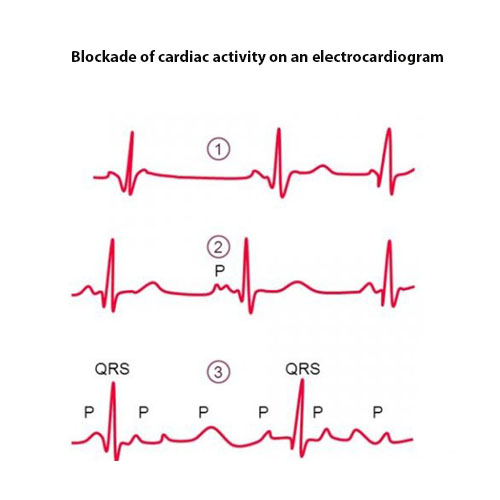
Inverted arrhythmia
Adverse disruption of the rhythm, accompanied by a reduction of atrium more than 300 times the minute, and ventricles - 200 times the minute. At the same time, the heart rate can reach 500 times per minute. Allocate various forms of the disease - paroxysmal, persistent, persistent and persistent. Each of them can meet with a hypertensive illness.
Recent studies have shown that atrial fibrillation develops in 5% of people after 60 years of age. It is precisely this category of the population that is included in the risk group for hypertension, so these two pathologies in the clinic often combine. The most dangerous is the permanent form of MA, which tends to go over to ventricular fibrillation more than the rest. Pathology also increases the risk of developing thromboembolism blood vessels and stroke.

Fibrillation of the atrium and ventricles.
A life-threatening condition in which chaotic, irregular and very frequent cardiac contraction develops. Anesthetics and ventricles work rashly, because of which the heart ceases to perform its functions. As a result, the whole body begins to feel the acute shortage of oxygen.
With hypertension, this complication along with stroke is one of the most formidable. It develops mainly in the last stages of the underlying disease. An independent resolution rarely occurs, therefore, ambulance is needed.
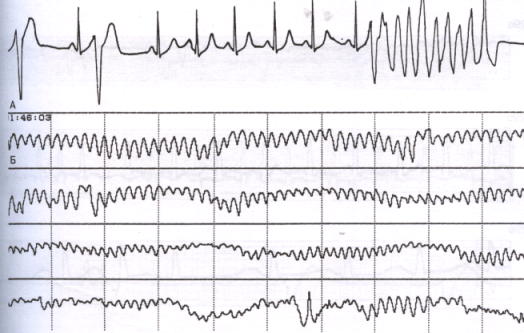
Diagnosis of hypertonic arrhythmia
The first place is electrocardiography . With its help in 90% of cases, any form of arrhythmia is determined. It is especially useful when the patient does not make specific complaints of heart rhythm abnormalities. ECG decryption helps to identify sinus tachycardia, blockade, crying, paroxysmal arrhythmia, and fibrillation of any localization.
Other methods of research can clarify the state of the cardiovascular system. They include:
- Echocardiography or ultrasound of the heart
- Holter monitoring
- Ultrasound of the thyroid gland
- Lipid profile
- Biochemistry and general analysis of blood
Additional diagnostic methods include transesophageal and intracardiac investigations using an echocardiograph or electrophysiological method. Also, if necessary, perform a test with physical activity, which must be prescribed in the absence of arrhythmia. Therefore, this variant of the diagnostics is not suitable for permanent forms of rhythm disturbance.
Treatment and prognosis for hypertonic arrhythmia
Much depends on the type of arrhythmia, because one thing is to prescribe a therapy for sinus tachycardia, and quite another - with flickering or fibrillation of the ventricles. Therefore, after setting the diagnosis, the most appropriate method of treating hypertonic arrhythmias is chosen
Medicinal treatment
Since rhythm disturbance has developed in the context of hypertension, those drugs are prescribed, which are aimed at preventing the aggravation of the course of the underlying disease. Such medicines are considered:
- ACE inhibitors;
- statins and sartans;
- diuretic substances;
- blockers of beta-adrenergic receptors and calcium channels;
- antiarrhythmic drugs.
These drugs are taken for a long time, which allows you to achieve a multiplier effect on the pathological processes occurring in the heart and blood vessels. Not all drugs are prescribed at once, but the most suitable combinations from the already proposed schemes of treatment of arrhythmia in hypertonic disease are selected. For this purpose, the cardiologist, who gives the necessary recommendations for taking medicines, is visited.
Surgical treatment
With arrhythmias, developed in the background of hypertonic disease, rarely when appointed. This is due to the fact that the patient, as a rule, is at an age and in such cases it is unsafe to lie down on the table. Also, multiple changes in the cardiovascular system, associated with hypertension, have become much widespread, which is almost impossible to solve during one operation. Therefore, surgical intervention may be appropriate for full blockade and some types of paroxysmal tachycardia. In other cases, adequate medical condition of the patient should be selected.
Video Breathing gymnastics for the treatment of hypertension and arrhythmia
Prevention of hypertonic arrhythmia
It can only consist in preventing the aggravation of the course of hypertonic disease, which will help reduce the likelihood of developing severe forms of heart rhythm disorders. For this, the first thing to do is to select an effective antihypertensive drug. Further on the background of the treatment of hypertension is recommended:
- to organize rational nutrition in order to reduce cholesterol in the blood, for which fatty meat and dairy foods should be replaced with seafood, fruits, vegetables, low-fat varieties of meat and dairy products;
- to refuse harmful habits (smoking, alcohol and toxic substances);
- to increase physical activity, for which one should choose the appropriate state of the sport (yoga, pilates or just regular walking in the fresh air).
- Avoid stressful situations that can both increase blood pressure and cause an arrhythmia attack, so in case of emotional stress it is best to have a calming remedy in advance.
Video Hypertension, arrhythmia and other diseases of the heart - causes and essence
Similar articles
For the effective treatment of hypertonic arrhythmias, the main cause must be eliminated – hypertonia. For this purpose, preparations from existing classes of antihypertensive drugs are used. These may be beta-blockers, angiotensin receptor antagonists, calcium antagonists, thiazide diuretics. It is also important to change lifestyle, reduce weight, abandon bad habits. Treatment of arrhythmia with hypertension is of secondary importance if it is not associated with severe hemodynamic disorders. For example, with sinus arrhythmia, extrasystoles, paroxysmal tachycardia, there is enough symptomatic therapy in the form of potassium, isoptin, antiarrhythmic drugs. Such forms of arrhythmia as flickering, trembling, and fibrillation require resuscitation because they are life-threatening.
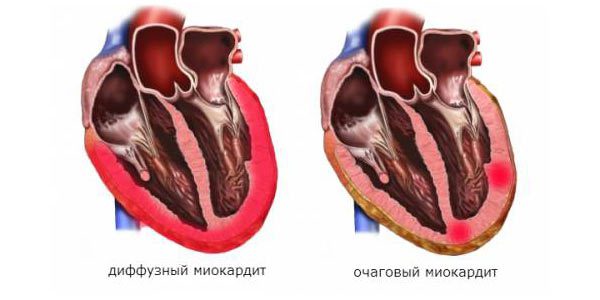
Among all cardiovascular pathologies, the most frequent complication of infectious diseases is myocarditis. Its prevalence is difficult to assess, since much depends on the occurrence of the underlying disease. If diphtheria accounts for an average of 25%, then ARVI rarely reaches 15%.

ECG (or electrocardiogram) is one of the most common and accessible research methods and demonstrates the details of the functioning of the heart in the form of a graphic image that reflects the electrical activity of the organ. This method is often used for the initial diagnosis of cardiac pathologies, is carried out as part of a comprehensive examination of the patient before presumed treatment or during preventive examinations.
