Preparations for bradycardia
This section presents preparations for the treatment of bradycardia, which are most often used to arrest an attack of rhythm disturbance. Only in some cases, drugs are used for long-term therapy of the disease.
Bradycardia is a kind of arrhythmia, in which the slowing of the heart rate is determined. Pathology can occur on its own, but most often it is caused by other diseases or by improper intake of certain medications.
In some cases, the bradycardia does not threaten anything, while in others it can lead to a sudden cardiac arrest. In an uncomplicated clinic, patients are prescribed medications, whereas a severe bradycardia is often eliminated by surgical intervention.
Video: Bradycardia | What to do
Drugs used to treat bradycardia
Normally, the heart rate in an adult is 60-90 beats per minute. A heart rhythm that is defined less than 60 beats / min is called bradycardia. In some cases, depending on the age and physical condition, a slow rhythm is determined in a person without any other pathological manifestations and then one speaks of physiological bradycardia.
Cardiac activity can slow down during deep sleep.
Older people are more likely to develop a slow heart rate.
There are also other causes of bradycardia, which sometimes lead to serious complications.
Causes of bradycardia
- Problems with the sinoatrial (CA) node, which is sometimes called a natural cardiac pacemaker.
- Problems with conduction pathways of the heart (electrical impulses are not conducted from the atria to the ventricles).
- Metabolic disorders such as hypothyroidism (thyroid disease by type of hypothyroidism).
- Damage to the myocardium during a heart attack or other heart disease (myocardial infarction, cardiomyopathy).
In addition, the cause of bradycardia can be:
- Substances with negative chronotropy
- Beta-blockers.
- Calcium channel blockers.
- Digoxin.
- Amiodarone.
- Clophelin.
- Verapamil.
- Hypoxia.
- Pain (can also cause tachycardia).
- Subcooling.
- Cushing's reflex (systemic response to increased intracranial pressure leading to increased impulse pressure, irregular breathing and bradycardia).
- Pericardial tamponade.
- Adrenal insufficiency.
- Severe obstructive jaundice.
- Pleural or peritoneal stimulation.
In rare cases, the infection causes a bradycardia, for example, typhoid, which can contribute to a relative slowing of the heart rate.
Symptoms of bradycardia
The heart rhythm, which is too slow, can cause insufficient blood flow to the internal organs. Especially from this the brain suffers, resulting in the following symptoms:
- Fatigue or severe weakness.
- Dizziness.
- Confusion of consciousness.
- Fainting or fainting condition
In the case of the presence of a primary or concomitant disease, their characteristic features may be determined.

Treatment and prevention of bradycardia
Treatment of bradycardia depends on the underlying cause. For example, if hypertension led to a slowing of the rhythm, the doctor can prescribe medications for bradycardia and make a treatment plan for the patient to lower blood pressure.
In severe cases, a pacemaker is implanted. It is a device that reproduces electrical impulses and helps the heart to work independently. Therefore, he is also called an artificial pacemaker.
Prevention of bradycardia is to organize a healthy lifestyle, which includes:
- Correct and high-quality food.
- To give up smoking.
- Full or maximum possible refusal of alcohol.
- Do not abuse drugs.
- Maintain weight within normal limits.
- Control and treatment of major diseases.
- Visit a doctor for regular examinations.
If a heart disease has previously been determined and the attending physician has drawn up a therapy plan, you need to take the medicine properly, and follow any other prescription of the doctor.
Essential preparations for bradycardia
There are recommendations of the American Association of Cardiovascular Diseases from 2015, which operate until they are replaced in October 2020.
Using the ACSI algorithm to control the bradycardia allows at the first stage to assess and provide assistance to a patient who has a symptomatic bradycardia. Its implementation begins with the establishment of the heart rate, which with a bradycardia is <60 bpm. Such violations are the cause of the disease state.
- Primary and secondary examination methods are used:
- If breathing is disturbed, measures should be taken to restore it.
- If the oxygen saturation is less than 94%, or the patient does not have enough air, an oxygen mask can be used.
- Blood pressure and heart rate are monitored.
- A standard 12-lead ECG is performed.
- The search and elimination of possible causal factors are carried out.
- Some questions should be answered that will help to decide whether the symptoms are caused by another disease or whether they are directly related to bradycardia:
- Are such signs or symptoms, such as hypotension, impaired breathing, dizziness, shock, persistent chest pain, shortness of breath, severe weakness or fatigue, severe altered mental status serious?
- Are the signs and symptoms directly related to a slow heart rate?
- Can there be another cause of symptoms in a patient other than a slow heart rate?
- A decision is made whether the patient has adequate perfusion. In the future, the tactics of treatment is determined by the severity of clinical manifestations in the patient:
- If perfusion is adequate, the patient is monitored and monitored.
- If perfusion is not sufficient, the following actions should be performed quickly:
- Preparations for percutaneous stimulation are under way. In such cases, it should not be postponed. If there is no pulse, stimulation is performed first.
- The possibility of administering atropine 0.5 mg, which can be repeated every 3-5 minutes to 3 mg or 6 doses, is considered.
- Adrenaline or dopamine is used, especially if the stimulation is not effective. Adrenaline from 2 to 10 mcg / min.Dopamine from 2 to 20 mcg / kg per minute.
Such actions should be performed as quickly as possible, since the patient may be in critical condition and need appropriate interventions: stimulation, atropine administration, dopamine infusion or adrenaline.
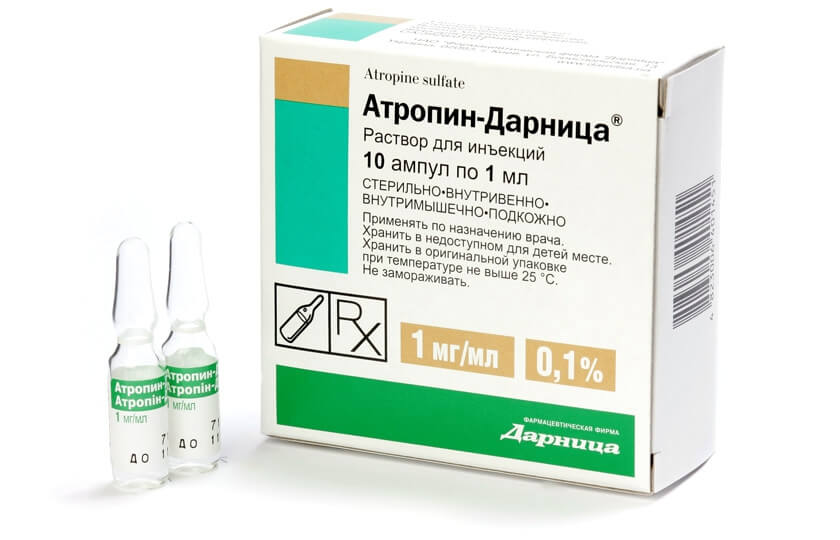
Drugs with sinus bradycardia
Sinoatrial blockade
With this pathology, the sinoatrial node can not independently generate electrical impulses or disrupt their distribution.When diagnosing ECG, there are usually no P waves and they are characterized by a slow rhythm:
- Wrong - narrow complexes with a frequency of 45-60 beats / min.
- Ventricular - wide complexes with a frequency of 30-45 beats / min.
Causes:
- Ischemia.
- Hyperkalemia.
- Vagotonia.
- Negative chronotropes.
Syndrome of weakness of the sinus node
Characterized by bursts of atrial tachycardia, alternating with periods of bradycardia, paroxysmal atrial flutter or fibrillation.
Causes:
- Sinoatrial or atrioventricular nodal fibrosis.
- Ischemia of the myocardium.
- Congenital heart defect.
The ECG can determine the blockade of the sinus node, sinus or atrial bradycardia with splashes of atrial tachycardia (usually atrial fibrillation).
Treatment
Pharmacological therapy is often the first line of treatment for sinus bradycardia, since it is the most accessible. The list of drugs used is shown in Table 1. It should be noted that drugs that increase the heart rate may worsen the course of the blockade inside the sinus node.
Table. 1
| Name of the drug | Act | Dosage | Pharmacokinetics | Comments |
| Atropine | Muscarinic antagonist of acetylcholine receptor | 0.5 mg intravenously (repeat every 3-5 minutes to 3 mg) | t½ 3-4 hours. ~ 50% is excreted through the kidneys | Applicable in the case of nodal blockade. Doses of <0.5 mg can paradoxically worsen the course of bradycardia. Contraindications: glaucoma, prostatism, ileus |
| Isoprenaline / isoproterenol | The alpha-1, alpha-2, beta-1 and beta-2-adrenoreceptor agonist | Begin with an infusion of 4 μg / min, then increase / decrease the amount by 1-10 μg / min, depending on the response | t1 1 min | Can not be used for a long time because of side effects (trembling, headache, etc.) |
| Adrenaline / adrenaline | Alpha and beta-adrenergic receptor agonist | Infuse 2-10 μg / min and look for an answer | t1 3 min, followed by a slower release (t1 10 min) | A useful remedy, especially if hypotension is a problem (because of the vasoconstrictor effect) |
| Dopamine | Dopamine and alpha-and beta-adrenoreceptor agonist | Infuse 4-10 μg / kg / min | t½ 2 min | Bolus injections can not be performed |
| Dobutamine | Beta-1 adrenoceptor agonist | Infuse 3-10 μg / kg / min | t½ 2 min | A useful remedy, especially if inotropic insufficiency is noted simultaneously with bradycardia |
| Theophylline | Adenosine receptor antagonist and phosphodiesterase inhibitor | 100-200 mg slow infusion | t1 4-24 hours | Rarely used to treat bradycardia. There are features of use at a different age, smoking, liver failure, interaction with drugs, etc. |
| Aminophylline | Adenosine receptor antagonist and phosphodiesterase inhibitor | 200-300 mg, slowly intravenous injection | Rarely used to treat bradycardia |
All medications should be used with caution in the presence of cardiac ischemia. t1 = elimination half-life.
Long-term treatment of sinus bradycardia is based on the correction of lifestyle, the exclusion or minimization of risk factors. It is especially important to stop smoking and drinking alcohol, eat right and maintain weight within normal limits.If all methods of eliminating rhythm disturbance do not give proper result and a high risk of sudden cardiac arrest is determined, then a pacemaker is implanted.
Drugs with bradycardia caused by problems with the AV node
If there is a disturbance in the conductivity through the pathology of the atrioventricular node (AV node), talk about atrioventricular blockade. The AV node may be faulty for various reasons and then the normal passage of electrical impulses from the upper chambers of the heart (atria) to the lower chambers (ventricles) is disrupted.
With all blockades of the atrioventricular node, it is excluded:
- Ischemia or myocardial infarction.
- Lyme disease.
- Myocarditis or endocarditis.
- Systemic lupus erythematosus (SLE).
In clinical practice, three degrees of atrioventricular blockade are considered. The least pronounced symptoms are observed at the first degree of AV blockade, and the heaviest ones at the third degree.
The first degree of AV blockade:
- Slow conduction through the AV node.
- On the ECG: PR interval> 200 ms.
- All atrial pulses are carried to the ventricles.
- Benign current.
The second degree of AV blockade, in which some atrial impulses are not carried out in the ventricles:
- Mobitz type I:
- AB-conduction defect in the node itself.
- On the ECG: re-extension of the PR until the P-wave is followed by the QRS complex.
- Usually it is asymptomatic and no specific treatment is required.
- Treatment is performed if symptoms develop or when the lower myocardial infarction develops.
- Mobitz type II:
- The conductivity defect is below the AV node.
- The cause may be a degenerative lesion: Leo's disease (Lenaigre-Leo syndrome), which is acquired by a complete heart blockade due to idiopathic fibrosis and calcification of the electrically conductive system.
- On ECG: constant PR with intermittent absence of QRS.
- The risk of progression to blockade of the third degree.
- Atropine is ineffective in blockade below the AV node.
- Continuous pacemaking is necessary if the disease manifests itself as severe symptoms.
- Blockade 2: 1:
- On the ECG: 2 P waves after each QRS complex.
- It can occur with digoxin intoxication or myocardial ischemia.
- Further electrophysiological tests are needed to determine the treatment strategy.
The third degree of AV blockade:
- Dissociation of the AB-node.
- Atrial pulses are not carried to the ventricles.
- On ECG: both P-waves and QRS-emission complexes can be present, but they arise independently of each other.
- Treatment is carried out as described below, although atropine is often ineffective, so a permanent pacemaker is installed.
- Myocardial fibrosis is the most common cause of the disease.
- Association:
- Deterioration of acute myocardial infarction.
- Syndrome of weakness of the sinus node.
- Mobitz type II.
- Blockade of the second degree or fascial blockade.
Diagnosis of bradycardia and heart block
Evaluation of patients with suspected AV blockade requires careful collection of medical history, life history, heredity analysis and possible risk factors. In addition, laboratory and instrumental research methods are carried out:
- Doctors use electrocardiography to detect and diagnose bradycardia / heart block. An electrocardiogram is an image of electrical tracking of cardiac activity.
- Since many episodes of bradycardia and cardiac blockade are not permanent, but arise with interruptions, the patient may be offered for some time to vilify a special device by the type of mobile telemetry. With this method of monitoring, cardiac activity is registered round the clock, which allows detecting abnormal rhythms that are not recorded by a standard ECG.
- The determination of cardiac troponins is carried out in acute cases, when there is a suspicion of coronary heart disease (which is often the cause of AV blockade).
AV blockade can be of three degrees of severity and in each case one or another type of therapy is used.
Treatment of bradycardia, which arose because of the blockade of the heart
It is performed with the aim of restoring atrioventricular conduction, for which pharmacological methods of action or an artificial cardiac pacemaker are used. Both methods can be used in extreme circumstances, when it is required to quickly remove an attack of bradycardia. There is also a long-term treatment of slow rhythm with AB blockade and it is usually based on the use of pharmacological drugs.
In acute cases with bradycardia against the background of AV blockade use:
- Atropine 0.5 mg intravenously, if necessary, the dose is repeated up to several times. The drug helps to eliminate bradycardia and cardiac output. Especially it is effective at blockade in the most atrioventricular node. If the disorder is somewhat distal, then the deterioration of the course of the disease may reverse.
- Isoprenaline (isoproterenol) - is administered at 5 μg / min. In acute coronary syndromes should be used with caution, since it can cause ventricular tachycardia.
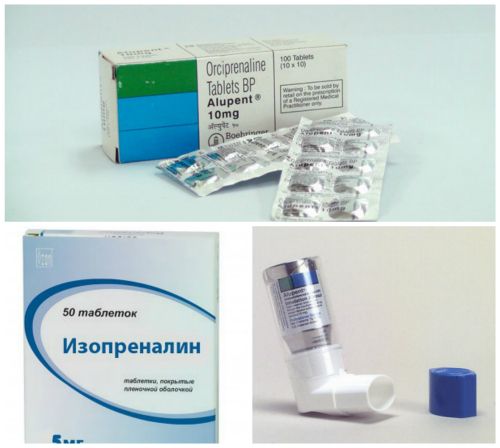
- Percutaneous or transvenous electrical pacing - appropriate instruments or preparations for administration are used. In both cases, an electric pacemaker is activated, which sends the heart of a certain strength currents that stimulate it to contract in a normal rhythm. An analgesic is used to reduce the painfulness of the procedure.
It is important that any drugs that can cause or aggravate the course of bradycardia on the background of the AV blockade, were abolished.
If the cause of the AV blockade is reversible, then the pacemaker is temporarily administered. In such cases, transvenous pacemaking is most often used and appropriate drugs are then given. If an AV block of a high degree is determined, then the patient's condition can only be improved by implantation of a pacemaker.
Long-term treatment of AV blockade with a pacemaker:
- AV blockade of the first and second degree, and also Mobitz type I - the pacemaker is only established in the presence of symptoms of the disease. Also the indication is the determination of wide ventricular complexes on the ECG.
- AV blockade of the second and third degree, and also Mobitz type II - patients are shown the implantation of a pacemaker. If Mobitz type II is defined with wide ventricular complexes on the ECG, the pacemaker is installed even in the absence of symptoms.
Drugs with bradycardia caused by hypothyroidism
Thyroid hormones have a direct effect on the work of the myocardium: they help to reduce and pump blood throughout the body. If there are not enough thyroid hormones, the heart rate may slow down too much. Also increases the risk of peripheral vascular resistance, reflecting the amount of pressure that the heart must create to circulate the blood normally.
There is also a link between hypothyroidism and elevated cholesterol. In addition, low thyroid hormone levels can cause insulin resistance, known as metabolic syndrome or "prediabetes," which in turn can lead to diabetes, obesity, high levels of homocysteine, and an increase in diastolic blood pressure. Together, all these factors contribute to the onset of heart disease.
The reasons given in patients with low thyroid hormone levels often contribute to development:
- High diastolic blood pressure.
- Bradycardia (slow heart rate).
- Shortness of breath (especially during exercise).
- Hypercholesterolemia.
- Increase homocysteine.
Sometimes weakly expressed symptoms of the thyroid gland, which are accompanied by low arterial pressure, are determined. Also, not all patients with hypothyroidism have a high cholesterol level. For this reason, when considering the diagnosis, predisposing factors should be considered.
Treatment of hypothyroidism and bradycardia
Since hypothyroidism is the main disease, against which bradycardia occurs, it is with his therapy that the process begins to improve the patient's well-being.
Low levels of thyroid hormones can occur for many reasons - starting with stress and ending with the toxicity of some drugs and iodine deficiency. Therefore, when it comes to treating hypothyroidism, some important points should be considered.
- Was the patient exposed to toxins? Sometimes it is enough to live near a farm on which the fields are treated with pesticides to cause dysfunction of the thyroid gland.
- What is the level of iodine? Iodine is the main building block in the formation of the thyroid hormone T4. In the body, the liver, kidneys and skeletal muscles are responsible for the transformation of T4 into its active form T3. Because T3 is an active thyroid hormone, it is important that the body has sufficient components, such as selenium, zinc and copper, so that the necessary transformations take place normally.
- Did you have to be stressed or had adrenal gland disorders? Like iodine, the adrenal glands also participate in the conversion of T4 to T3. If there is a high level of cortisol, T4 can be converted into an inactive hormone of reverse T3 (rT3), leaving the less active T3 available for exposure to cells. To assess the state of the adrenal gland, a doctor may recommend testing the index of adrenal tension using the formula of R.M. Bayevsky. Also, the level of cortisol can be measured during the day, which makes it possible to evaluate the function of the adrenal glands.
- What is the level of iron? Since many symptoms of hypothyroidism are similar to those caused by iron deficiency anemia, it is important to exclude low iron levels. Moreover, hypothyroidism can lead to an inadequate amount of acid in the stomach, which leads to poor absorption of nutrients, including iron and vitamin B12. The low iron content in the body also reduces the conversion of T4 to T3 and may increase levels of TSH.
- Is there enough vitamin D? Vitamin D deficiency is associated with the degree and severity of hypothyroidism. Thus, you can ask the attending physician to check the level of vitamin D.
- Is there gluten intolerance? An increased correlation is established between those who have an autoimmune thyroid disease, such as Hashimoto's disease, and celiac disease (an autoimmune disease in which the use of gluten causes damage to the cells of the small intestine). Therefore, if necessary, screening for celiac disease and intolerance to gluten are performed.
Hypothyroidism is treated with replacement doses of thyroid hormones. Synthetic forms of these hormones are available:
- Levothyroxine (Synthroid, Levothroid, etc.)
- Lytironin (Cytomel, Triostat)
- Lyotriks (Thyrolar)
- Thyroid gland.

With timely treatment, the changes that contribute to the onset of bradycardia are reversible.
Drugs with bradycardia caused by Lyme disease
Lyme disease is caused by the bacteria Borrelia burgdorferi, which are transmitted to people through a bite from infected ticks. Symptoms can occur 3-30 days after the bite and can be expressed, depending on the stage of infection. In some cases, signs appear several months after the bite.
Symptoms of Lyme disease
Early signs of the disease include fever, chills, headache, fatigue, pain in the muscles and joints, swollen lymph nodes - all this is common with the flu. In 80% of cases, the rash is one of the first symptoms of the disease.
Without treatment, symptoms can progress. In particular, there may be:
- Severe headache or stiff neck.
- Rash on other parts of the body, except the place of bite.
- Arthritis with severe pain in the joints and swelling, especially in the knees.
- Loss of muscle tone or "lowering" of one or both sides of the face.
- Irregular heartbeat.
- Shooting pain, numbness or tingling in the hands or feet
Stages of Lyme disease development
- Localization: flu symptoms such as fever, chills, headache, swollen lymph nodes, sore throat and usually a rash that has a bullish eye, or evenly round and red in color and at least 5 centimeters in diameter.
- Earlier spread: flu symptoms that now include pain, numbness of weakness in the arms and legs, changes in vision, heart palpitations and chest pain, rash and facial paralysis (Bell's paralysis)
- Later spread: this can occur in weeks, months or years after the tick bite. Symptoms may include arthritis, severe fatigue and headaches, dizziness, sleep disorders and mental disorders.
Treatment of Lyme disease
Antibiotics are used to treat the early stage of Lyme infection. Patients usually take:
- Doxycycline for 10 days to 3 weeks or
- Amoxicillin and cefuroxime for 2-3 weeks.
- In 90% of cases, the antibiotic helps to cure the infection. If this is not the case, patients may receive other antibiotics either in tablets or for intravenous administration.
With the early spread of Lyme disease, which can occur when the infection is not treated, oral antibiotics are recommended. Indications for their reception is the presence of such symptoms as facial paralysis and abnormal heart rhythm (bradycardia). Intravenous antibiotics are recommended if a person has meningitis, inflammation of the meninges and spinal cord or more serious heart problems.
When a late stage disease is reached, the patient can take oral or intravenous antibiotics. Patients with protracted arthritis undergo a standard treatment regimen prescribed for arthritis.
Drugs that cause bradycardia
There are drugs that, if not properly taken, can cause a slow heartbeat. Among them, the following are most often used.
Agalsidase (Agalsidase)
The drug is used for enzyme replacement therapy.
The most common side effects are chills, fever, heat or cold feeling, shortness of breath, nausea, swelling of the face, mouth and throat, redness, headache, vomiting, tingling, fatigue, itching, aching pain, high blood pressure, chest pain , sore throat, abdominal pain, dizziness, fast heart rate, nasal congestion, diarrhea, muscle pain, back pain, pallor, slow heart rate, hives, low blood pressure, face swelling, rash and drowsiness.
Bisoprolol
Refers to beta-blockers of selective action. With the right appointment it is possible to undergo treatment with minimal side effects or without them at all.
The most common side effects are abdominal cramps, diarrhea, dizziness, fatigue, depression, headache, nausea, impotence, slow heart rate, low blood pressure, numbness, tingling, cold extremities, sore throat and shortness of breath.
Calfactant
It is used to prevent the development of distress syndrome in premature infants. Most often does not cause side effects, but sometimes it can contribute to the development of bradycardia and other signs of impaired internal organs.
The most common side effects: blue-eyed child, respiratory obstruction, slow heart rate, surfactant reflux into the endotracheal tube and the need for artificial ventilation.
Dexmedetomidine (Dexmedetomidine)
A sedative, which should be taken and canceled strictly according to the recommendations of the doctor, otherwise there may be significant side effects.
The most common side effects are low blood pressure, slow heart rate, dry mouth.
Iopromide (Iopromide)
An X-ray contrast substance, which is used for various diagnostic studies, most often by radiography.
The most common side effects are shock, coma, stroke, cerebral edema, convulsions, abnormal heart rhythm, cardiac arrest, heart attack, heart failure, slow heart rate, blue skin, low blood pressure, shortness of breath, pulmonary edema, respiratory failure and aspiration.
Remifentanil (Remifentanil)
Opioid analgesic, which has a powerful, albeit short action. Often combined in admission with other sedatives.
The most common side effects are nausea, vomiting, pruritus, headache, increased sweating, shaking, dizziness, low blood pressure, slow heart rate, respiratory depression, muscle stiffness, chills, redness, a feeling of heat or heat.
Ropivacaine
Local anesthetic, which is mainly used in surgery. Incorrect use of the drug can lead to depression of the central nervous system and the heart muscle.
The most common side effects are low blood pressure, nausea, vomiting, slow heart rhythm, fever, chills, pain, postoperative complications, nasal congestion, decreased all kinds of sensations, anemia, tingling, headache, itching and back pain
Verapamil
The drug is often used to stop tachycardia, so if an overdose can be too slow heart rate.
The most common side effects are constipation, headache, respiratory infection of the upper respiratory tract, dizziness, fatigue, edema in the extremities, nausea, increased liver fermentation, slowing of the heart rhythm, tingling and low blood pressure.
In some cases, the manifested high toxicity of drugs is stopped by certain treatment regimens, which reduce the severity and risk of side effects. Details are indicated in the table below.
Table. 2 Options for treatment of bradycardia caused by the toxic effects of certain drugs.
| The drug that causes bradycardia | Treatment | A comment |
| Beta-blocker | Glucagon |
Antidote of the first line. 2-10 mg bolus, then 2-5 mg / h infusion. |
| Inotropes: adrenaline, dobutamine, isoprenaline |
Competitive beta receptor agonists. High doses are often required to overcome the effect of beta blockade. |
|
| Calcium channel blockers | Intravenous administration of calcium |
Antidote of the first line. Partially overcomes calcium blockade Calcium chloride or calcium gluconate can be given as boluses or for infusion control. |
| Glucagon | Can be used as a bolus or infusion: 2-10 mg bolus, then 2-5 mg / h infusion. | |
| Digoxin | Digoxin-specific antibodies (Fab fragments) | Antidote of the first line. Allergenic and expensive. Only for use in life-threatening arrhythmias attributed to digoxin. |
Video: Pills from pains in the heart
