Antidromic tachycardia
Author Ольга Кияница
2017-11-14
Antidromic tachycardia is found much less frequently than orthodromic. Its occurrence is mainly due to Wolf-Parkinson-White syndrome (WPW syndrome), a congenital anomaly characterized by the presence of an additional pathway. It is this path that underlies the appearance of antidromic tachycardia.
In the absence of WPW syndrome, in almost 90% of cases, such supraventricular tachycardia are diagnosed. as an atrioventricular-nodular reciprocal tachycardia and orthodromic tachycardia, combined with a crisp additional pathway.
Video WPW (Wolff-Parkinson-White Syndrome) Animation Video
Description of antidromic tachycardia
Paroxysmal atrial tachycardias, to which the antidromic form of rhythm disturbance belongs, are associated in their appearance with the mechanism of reentry - the re-occurrence of the excitation wave. The pulse circulation is mainly carried out in a closed loop within an atrioventricular node or sinus node. Secondary channels of an excitation wave, called the Kent bundles, and normally absent, can also be formed between the atrium and the ventricles.
Additional paths for carrying impulses are hidden, then the emerging tachycardia is denoted as orthodromic. It is also possible to clearly manifest additional paths, that is, well diagnosed using an ECG. This kind of education is characteristic of the WPW syndrome, in which both orthodromic tachycardia and antidromic occurs.
Circulation of the excitation wave with antidromic tachycardia passes through the atrium contour - an additional pathway - the ventricles - the atrioventricular node - the atrium.
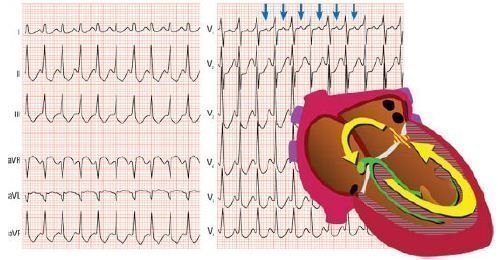
The relatively rare occurrence of antidromic tachycardia is associated with the fact that through the atrioventricular node the excitation wave passes much more slowly in the orthodromic direction. This creates favorable conditions for the start-up of the mechanism of re-entry.
The presence of several Kent bundles contributes to the simultaneous occurrence of an orthodromic and antidromic tachycardia in one patient.
Several additional pathways can be detected in the WPW syndrome, which form the basis of the formation of pre-excited tachycardia. With this form of rhythm disturbance anterograde and retrograde conduction of impulses is observed. Often pre-anxious and antidromic tachycardia are considered to be one and the same disease, since there are no obvious differences in ECG-signs and treatment tactics are almost identical.
Symptoms of antidromic tachycardia
The onset of the disease is not related to age, therefore it can be determined even in newborns. Any disorder of atrioventricular conductivity is a common provocation of the pathology development. This can be blockade or extrasystoles.
During paroxysms of tachycardia, especially with their frequent occurrence, hemodynamics within the heart is disturbed.A similar disorder affects the state of the heart chambers, which expand and begin to contract with insufficient force.
The clinical picture of tachycardia depends on a number of factors: the duration of rhythm disturbance, the frequency of its occurrence, and the presence of additional cardiac pathologies. In itself, antidromic tachycardia in WPW syndrome is not dangerous, but with a significant violation of hemodynamics on its background may develop life threatening tachyarrhythmias - fibrillation, throbbing of the ventricles / atrium.
Causes of antidromic tachycardia
The main cause of antidromic tachycardia is WPW syndrome, which is a hereditary pathology of the heart. In this case, the severity of the syndrome often depends on the presence and quantity of additional paths, called the Kent bundles. A wave of excitation passes through it, passing the atrioventricular node.
Kent's bundle is an abnormal formation of conductive fibroids that is detected between the ventricles and the atria. It was opened by the English physiologist Kent.

From a biochemical point of view, the development of WPW syndrome, and in particular antidromic tachycardia, is associated with gene mutations.
Diagnosis of antidromic tachycardia
The electrocardiogram defines widespread deformed ventricular complexes, as opposed to the narrow QRS that are formed during orthodermic tachycardia. In this case, the teeth P beyond the wide ventricular complexes are practically not determined.
Occurrence of tachyarrhythmia in usual cases is preceded by atrial extrasystole.
The peculiarity of antidromic tachycardia is the determination of the expressed delta wave on an electrocardiogram.There are also other signs that resemble ventricular tachycardia. Similar characteristics are associated with the fact that the ventricles are excited by passing the impulse along additional paths.
Treatment and prevention of antidromic tachycardia
In this pathology, firstly, medication therapy is prescribed, which includes the following drugs:
- sotalol;
- procainamide;
- quinidine;
- digoxin;
- Mexille;
- adenosine;
- verapamil
It is not recommended to use preparations of the following groups of arrhythmias in the treatment of antidromic tachycardia: cardiac glycosides, beta-adrenergic blockers, calcium channel blockers. This is due to the fact that they can increase the refractory period and thereby worsen the condition of the patient with an increase in the frequency of heart rate.
The ineffectiveness of medication treatment is an indication of a catheter ablation, during which additional paths are crossed.
Prevention is to prevent the development of tachycardia attacks, for which the same drugs or more radical surgical methods of treatment are used.

Здравствуйте!
Есть вопрос. В лечении антидромной тахикардии в Вашей статье указаны соталол, дигоксин, верапамил и следующим пунктом противопоказания – эти же классы препаратов. Прошу обосновать такое.
Спасибо.