Angiopathy
Author Ольга Кияница
2018-03-05
Angiopathy (AP) is characterized by vascular damage, often of small and middle caliber, as a result of which the corresponding clinic develops. Arises on the background of various diseases (diabetes mellitus, hypertension, due to injury), so it is considered a complication.
The prolonged course of angiopathy threatens the appearance of chronic disorders in the blood supply system, which leads to a disorder of the activity of various organs and parts of the body.
Examination of patients with angiopathy plays an important role in the correct diagnosis, since it is important to determine the underlying cause of the pathology development. The AP course may be more or less pronounced, but appropriate treatment must be performed. Otherwise, the tissues that bleed the affected vessels begin to die.
Video Hypertonic angiopathy of the retina. What is it and what is it dangerous?
What is angiopathy?
In normal condition, small caliber vessels are elastic and free for blood flow. In angiopathy, their structure is broken, as a result of which they become brittle, with thick walls, in some cases partially or completely overlaps the lumen of the vessel. All this contributes to a change in the normal circulation of blood, which causes blood supply to tissues and organs.
When angiopathy is most often amazed:
- Lower extremities
- Retinal eyes
- Head brain
- The kidneys
It is precisely in these organs and parts of the body that the vessels of the small caliber are most concentrated. If the structure of a small part of the capillary mesh is broken, the slight signs of the disease develop rather quickly, and after the time is more pronounced and clinically unfavorable.
Predisposing factors leading to angiopathy:
- Disturbance of the nerve regulation, expressed in the change in the tone of the vessels (their persistent expansion, that is, dilation, or excessive narrowing, that is, spasm).
- The presence of abnormal proteins in the blood that impregnates the vascular walls, thus changing their structure.
- Increased pressure in the vessels, which has a negative effect on the vascular wall.
- Inflammation that lasts for a long time.
Angiopathy is more often defined in diabetes mellitus, as this disease is very common today. Other forms of the disease are no less complex and dangerous in their development, therefore there is such an opinion:
"Angiopathy develops suddenly and leads to severe consequences"
A bit of statistics:
- Defeat of kidney vessels in 60% of cases develops against a background of diabetes, and in 40% - arterial hypertension.
- 80% of patients with angiopathy have bad habits, they are over 50 years old or they have other risk factors.
- In patients with diabetes, angiopathy occurs after 10-15 years. Development of the underlying disease.
- In 35-40% of patients of working age, angiopathy is detected in the vessels of the heart.
- Depending on the clinical form of the AP, the complication in the form of angiopathy of the brain occurs in 5-75% of cases.
Reasons
Angiopathy is a secondary pathology in 90% of cases, as it develops against other diseases. The remaining 10% are defined as primary angiopathy, which is an independent pathological condition.
Main causes of AP:
- Atherosclerosis.
- Hypotonic angiopathy. It is associated with decreased peripheral vascular tone.
- Hypertensive angiopathy. It develops due to increased pressure in the peripheral vascular bloodstream.
- Traumatic angiopathy . Arises due to compressive damage to various parts of the body and other injuries.
- Diabetes mellitusCauses damage to capillaries in various organs due to the deposition of sorbitol and fructose in the vessels.
- Amyloidosis Bound with circulating blood in an abnormal protein that has a chronic intoxication to organs and tissues.
- Connective tissue diseases (lupus, rheumatoid arthritis).
- Autoimmune diseases. Angiopathy can be complicated by scleroderma, sclerotic vasopatiya, polyarthritis.
- Diseases of the blood. In diseases such as thrombocytosis, leukemia, polycythemia, an increased number of blood cells is observed, which also has an adverse effect on the walls of the vessels.
In addition, angiopathy may be associated with disorders of the spinal cord and brain, the autonomic and peripheral nervous system. Similarly, it also often affects the structure and function of the capillary system.

Risk factors that contribute to the development of angiopathy:
- The presence of bad habits (smoking, drinking alcohol).
- Disorders of the metabolic process.
- Unfavorable working conditions.
- Hereditary diseases.
- Age 50 and older.
The more the risk factors are determined in the patient, the more severe and more pronounced the underlying disease and its complication in the form of vascular damage.
Species
Angiopathy is divided into clinical forms, taking into account the causes of the disease, the size of the lesions and their localization.
Allocate the following types of angiopathic lesions:
- because of:
- diabetic;
- hypertonic;
- hypotonic;
- traumatic;
- toxic;
- neurogenic;
- amyloid
- by localization:
- retinopathy (affects the retina of the eye);
- nephropathy (the pathological process affects the kidneys);
- angiopathy of the extremities, most often lower ones;
- angiopathy of the vessels of the brain;
- angiopathy of other organs (intestines, heart, lungs).
- by size of defeat site:
- microangiopathy (affect vessels of small caliber, that is, capillaries);
- macroangiopathy (in the pathological process involves the middle and large vessels, in such cases their atherosclerosis is additionally observed).
One patient may have several clinical forms of angiopathy (for example, damage to the retina of the eye, kidneys and lower extremities, which is characteristic of the diabetic form of angiopathy). Such multiple vascular damage is observed in 65% of patients with AP.
In some cases, temporary damage to the vessels is determined, which, if properly monitored, may not require specific treatment. In particular, careful attention to capillaries is required in the following cases:
- The patient was exposed to oxygen starvation.
- The birth of a child was accompanied by complicated or severe childbirth, after which angiopathy was detected.
- During pregnancy, angiopathy, caused by an increased vascular load, is determined.
Diabetic angiopathy
A typical angiopathy develops against a background of diabetes mellitus, when the capillary channel changes with the background of an increased amount of sugar in the blood. After the capillaries, the defeat affects larger vessels, which, after prolonged course of the illness, leads the patient to severe disability.
With diabetes, glucose levels often rise above 6 mmol / L, which contributes to the deposition of various vessel derivatives on the walls of vessels.As a result, the vascular walls thicken, the lumen of the vessel narrows, their brittleness rises, which subsequently leads to the extinction of soft tissues.
Diabetic angiopathy is most often expressed in:
- angiopathy of the lower extremities (diabetic foot);
- retinal angiopathy;
- nephropathy.
The disease is dangerous because of its consequences, because in diabetic foot, the affected limb is often amputated. Involvement in the pathological process of larger vessels leads to heart attacks, stroke, heart failure.
Video Diabetic Angiopathy: Symptoms, Diagnosis, Treatment
Hypertensive angiopathy
The high pressure in the circulatory system results in less severe consequences than diabetes mellitus. In the process of developing hypertension, vascular endothelium is damaged, as high pressure constantly affects it. As a result, the muscle layer begins to hypertrophy, which in the future leads to fibrosis.
Blood circulation is complicated, multiple sites of narrowing and even occlusion of vessels appear.At the same time, the blood pressure remains high, which in severe cases leads to greater or lesser hemorrhages.
With hypertonic angiopathy, it is most often amazed:
- retina of the eye;
- brain vessels;
- kidney arteries;
- coronary vessels of the heart.

Hypotonic angiopathy
The disease mainly affects the peripheral pathway, which, due to the reduced vascular tone, begins to overflow with blood. This leads to an increase in the permeability of the walls of the vessels, because of which in the lumen of capillaries accumulate form blood elements. This is a prerequisite for the formation of blood clots and edema. Similar changes are more often observed on the lower extremities, although when the disease progresses, the vessels of other parts of the body are subject to change.
Hypotonic angiopathy can go into hypertension, because prolonged stretching of the vessels leads to a reverse reaction - the vascular tone increases, but due to the formed rigidity of the vessels and deposits in their walls of calcium, prerequisites for the development of hypertonic disease are created.
The occurrence of hypotonic angiopathy is most often accompanied by:
- damage to the retina;
- brain vessels;
- change in the color of the skin.
For example, a patient can determine the cyanotic tint of the skin of the nose, ears, cheeks, chin. With a disturbance of blood circulation in the brain, vegetative disorders, as well as dizziness, can be developed in combination with headaches. At the retina at this time, arterioles and venules are also commonly observed.
Traumatic angiopathy
Depressing injuries to the chest, the skull leads to a very sharp increase in blood pressure. As a result of such a defeat, light patches are formed on the retina, in addition some vessels are clogged up. All this leads to deterioration of vision. When rendering timely medical care, the condition can be improved, but most of the time it is not possible to restore vision completely.
Clinic
The first degree of angiopathy may be asymptomatic and in such cases minor changes in the retina of the eye may be detected, which must necessarily lead to an explanation of the cause of the development of the pathological condition.
Typical complaints of angiopathy:
- Vision worsened (the patient sees cloudy pictures).
- Flashing stars can start before your eyes.
- The color sensation is also violated.
Other symptoms are associated with damage to the vessels of the internal organs and lower extremities:
- Feelings can be felt in the legs.
- Convulsion states develop.
- When exercising, often there is an intermittent lull.
- In the feet and hands there is a feeling of tingling or wrong perception.
- Small nasal hemorrhages may develop, and blood in the stool and urine is often determined.
Thrombotic microangiopathy is a characteristic symptom of dystrophy and tissue microchondensis, which manifests itself in every erosion and ulceration.
Clinical determination of blood flow disturbances must be supplemented by laboratory and instrumental studies, which will allow for a more accurate diagnosis and effective treatment.
Diagnostics
After the definition of clinical manifestations, a comprehensive examination of the patient is mandatory. To do this, various methods of research are used that assess the functioning of the internal organs, the nervous system, the state of the vascular bed.
The main way of determining the signs of arterial microangiopathy is to conduct ophthalmoscopy. For this purpose, an ophthalmologist visits the eye and examines the following disorders:
- capillaries are narrowed;
- vessels often cross, there is a crying of arteries and veins;
- expansion expansion of the capillary mesh;
- hemorrhagic hemorrhages are most often point-blank;
- the formation of small blood clots.
In addition, the following studies may be conducted:
- angiography;
- dopplerometry;
- duplex scan;
- magnetic resonance imaging.
The definition of vascular lesions with a maximum probability of development of complications is considered an indication for carrying out of the specific therapy, which is selected on an individual basis.
Treatment
Much depends on the clinical form of the disease, so various specialists are involved in the treatment of angiopathy:
- Vascular surgeon or general surgeon - angiopathy of the lower extremities.
- Neuropathologist - angiopathy of the brain.
- The therapist or nephrologist is a defeat of the vessels of the internal organs, for example, the kidneys.
- Cardiologist - diseases of the cardiovascular system.
The direction of medication therapy largely depends on the clinical form of angiopathy and the underlying disease, on the background of which it developed.
- With diabetes, it is important to maintain glucose levels within acceptable limits so that vascular lesions do not develop.
- The presence of hypertonic disease involves controlled use of antihypertensive drugs.
- Definition of atherosclerosis forces to adhere to dietary nutrition, permissible physical activity, treatment / prevention of disturbed metabolic processes.
In most cases, drugs from the following pharmacological groups are used:
- Anticoagulants Helps to treat and prevent thrombosis.
- Angioprotectors. The action of drugs is aimed at protecting the walls of the vessels.
- Metabolic substances. Mprove exchange processes.
Additionally, all measures should be taken to eliminate unmodified risk factors, that is, those that are capable of being changed.
Forecast and prevention
In most patients (about 85% of cases) who adhere to medical recommendations, the disease progresses poorly and does not contribute to the development of severe complications.
In malignant course of the main disease (hypertension, diabetes), in 99% of cases, angiopathy also occurs unfavorably. In such cases, blindness, renal insufficiency, or necrosis of the tissues develop. Therefore, the earlier the treatment is started, the greater the chances of maintaining health.
Similar articles

In some diseases, complications such as angiopathy of the retina occur. It significantly worsens the quality of life of the patient, and sometimes can lead to disability. Therefore, it is very important in such cases to undergo an accurate diagnosis and timely therapy.
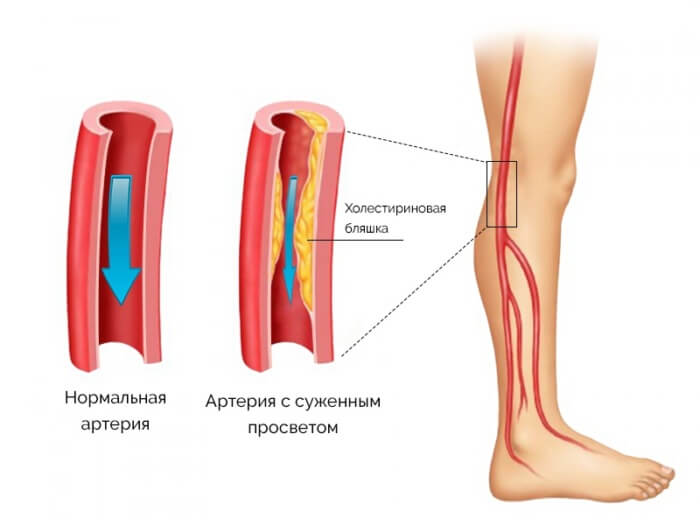
The group of vascular diseases includes angiopathy of the lower extremities, which is associated with impaired blood circulation and the structure of the vascular network of the legs. The disease can last for a long time and without severe symptoms. Trophy of trophism of tissues causes various complications, therefore full diagnostics and rapid treatment of the disease is required.

Как только маме поставили диагноз – диабет, я начала борьбу за улучшение ее качества жизни. Знаю, как при этой болезни страдают сосуды, поэтому, к комплексу мер, прописанных эндокринологом, попросила добавить препараты, улучшающие работу сосудистой системы. Врач рекомендовал Вазаламин, как наиболее безопасный препарат, совместимый с остальными лекарствами. Надеюсь, что действие цитаминов улучшит кровоснабжение тканей, предотвратит развитие ангиопатии.